What Is a Living Will?
A living will is a legal document that states your wishes for end-of-life medical care in case you cannot speak for yourself due to severe illness or incapacity. It’s helpful if you plan to undergo surgery, have a chronic condition, or work in a high-risk profession.
You can use it to dictate what life-saving interventions you want. For example, you can request that doctors implement or withhold resuscitation, mechanical ventilation, or tube feeding. A living will can also record your desired ways to manage pain. Without a living will, your nearest relatives, as determined by state law, will be responsible for these important healthcare decisions.
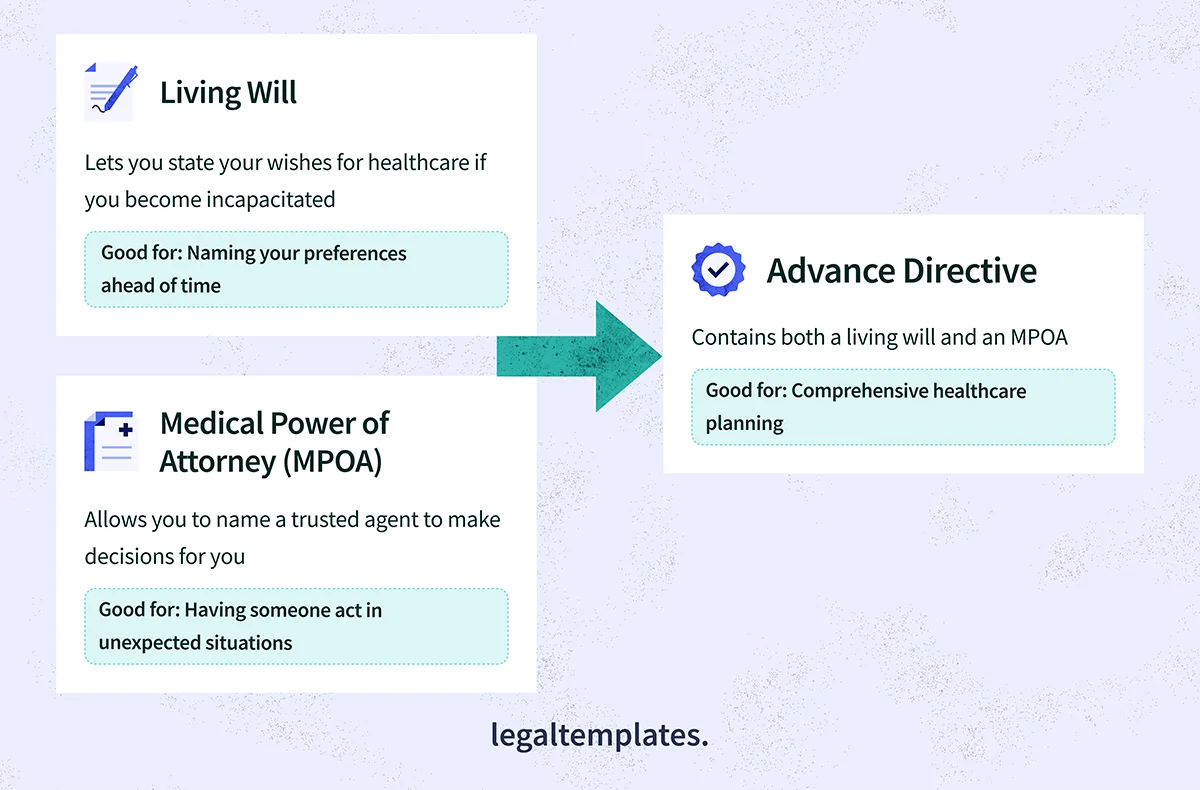
A living will is part of an advance directive, which is a broader medical document. An advance or health care directive contains both a living will and a medical power of attorney (MPOA). An MPOA appoints an agent to make healthcare decisions on your behalf when you cannot do so yourself.
How to Make a Living Will
If you’re wondering where you can get a living will form, you’ve come to the right place. Our guided template helps you create a concise document communicating your wishes to relevant parties. Explore how to make a living will without a lawyer below.
Step 1 – Add Your Information
Add your information as the living will’s author. Include your name, address, and contact details to make it clear you’re writing the living will for yourself.
Step 2 – Decide on Life-Prolonging Treatment
Decide how you want doctors to treat you during a critical medical emergency. Consider whether you would like to be kept alive by life-sustaining treatments or otherwise allow natural death to occur. On the form, you can list your preference in three main cases:
- A terminal condition (an injury or illness where death is imminent)
- A persistent vegetative state (a condition where you are unresponsive and unconscious for an extended period)
- An end-stage condition (an advanced and incurable condition where you will continue to deteriorate until you die)
For each decision, decide whether you want doctors to try and extend your life through any means necessary, and initial your preference on the form. Even if you choose against life-saving measures, you can still specify that you want to receive palliative care, which includes treatment to ease your pain and allow a peaceful death.
Step 3 – Elect Organ Donation Preferences
While optional, you can use your living will form to dictate your organ donation preferences. Make the following choices on your form:
- Which organs you want to donate
- What purposes your organs can be used for
- Whether you give your body for an anatomical study
- Any limitations on your organ donation
Step 4 – Nominate a Health Care Surrogate
Nominate a health care surrogate who can help ensure that medical professionals follow the instructions in your living will. Choose someone you trust and who’s willing and able to act when you cannot provide express consent yourself.
Step 5 – Include Additional Instructions
Note any additional end-of-life preferences, such as your wishes if you’re pregnant, your preferred care facility, and any spiritual or ritual rites you want performed.
Step 6 – Sign & Obtain Notarization
Sign your name to confirm your living will declaration. Be sure to sign before witnesses and a notary public if your state requires these parties to be present.
Some states only require witnesses, while others require witnesses and notarization. Depending on your state, you may be able to get the signature of witnesses or a notary public. Below, you can review your state’s signing requirements to ensure your document is legally valid.
| State | Witness Requirements | Notarization Requirements | Statute |
|---|---|---|---|
| Alabama | Two witnesses | n/a | AL Code § 22-8A-4 |
| Alaska | Two witnesses | Can replace the witness requirement | AK Stat § 13.52.010 |
| Arizona | One witness | Can replace the witness requirement | AZ Rev Stat § 36-3261 |
| Arkansas | Two witnesses | Can replace the witness requirement | AR Code § 20-17-202 |
| California | Two witnesses | Can replace the witness requirement | CA Prob Code § 4701 |
Do Any States Not Recognize Living Wills?
Massachusetts and Michigan don’t recognize living wills, so they are not legally binding. Even in these states, creating one can provide guidance for family members and medical professionals on the patient’s wishes.
Step 7 – Circulate Copies
Circulate copies to the appropriate parties so your wishes are properly understood. Without sharing the document upon completion, your family members or healthcare providers may not know your medical preferences regarding life-sustaining and end-of-life care. Ensure the following people and entities get a copy of your living will:
- Your primary care physician
- Your local hospital
- Any agents or healthcare powers of attorney
- Your health insurance company (if required)
- Your chosen family members and friends
Living Will Sample
View a living will sample to understand what it looks like. Then, use our free printable living will form to create your own. Download in PDF or Word format.
Living Will vs. Last Will
A living will specifies medical care preferences, while a last will distributes assets after death. A last will is an important end-of-life document to ensure your assets go to chosen beneficiaries. It also helps you settle other matters after death, like naming a guardian for your minor children.
Complete Your Estate Planning
Creating a living will and last will are just some of the steps in the estate planning process. Review our estate planning checklist to get your affairs in order.
Living Trust vs. Living Will
A living will is a medical document that clarifies end-of-life care and helps you ensure your medical wishes are followed, while a living trust helps you manage assets. You can create a living trust to control cash and property during your life. When you die, the assets will go to the named beneficiaries and avoid probate, creating an easier transition for your loved ones than using a traditional last will.
Living Trust vs. Last Will
Read about the differences between a living trust and a last will.